Post-traumatic stress disorder (PTSD) is a debilitating
mental anxiety disorder that develops after an individual experiences or witnesses a traumatic, tragic, terrifying or life-threatening event. People suffering from PTSD experience flashbacks to the traumatic event and a sensitivity to emotional or mental triggers that remind them of the experience, causing negative changes in their lifestyles and an inability to achieve normal goals or objectives.
7.7 millionAmerican adults have PTSD
1 out of 3people seeking treatment for substance use disorders have PTSD
65 percentof people with PTSD have a co-occurring substance use disorder
8 percentof Americans develop PTSD at some point in their lives
Events that lead to PTSD include war or military combat, accidents, physical or sexual assault, abuse, natural disasters, terrorist attacks, bombings, and events in which individuals are injured. Among those with PTSD,
co-occurring disorders are frequent, as high rates of combinations of depression and other anxiety disorders with substance addiction are usually found in these individuals.
For people with PTSD, a co-occurring substance use disorder can be extremely harmful. People with PTSD often experience problems with their interpersonal relationships, health and everyday functions. Combine this with a substance use disorder, and these difficulties are only amplified.
PTSD sufferers may use substances to “
self-medicate” as a way to treat symptoms such as isolation, sleep disturbances and emotional numbness. Unfortunately, using substances to alleviate PTSD symptoms provides only temporary relief while intensifying the negative effects and symptoms that stem from PTSD.
Nicholas Stefanovic, a former Marine who completed two tours of duty in Iraq and Afghanistan, began feeling the effects of PTSD when he returned to the United States in 2006. He turned to prescription opioids to deal with his symptoms.
“I started using [OxyContin] because it was like a miracle drug for me,” Stefanovic told DrugRehab.com. “[The drugs] immediately fixed my problems.”
People with PTSD most commonly use alcohol to alleviate their symptoms, with about 52% of men and 28% of women with PTSD meeting the criteria for alcohol abuse.
He knew that misusing opioids could cause another set of problems. He didn’t care. He had no plans for the future anyway, he said.
“I was not suicidal, but there were times when I didn’t care if I lived or died,” Stefanovic said.
People with PTSD most
commonly use alcohol to alleviate their symptoms, with about 52 percent of men and 28 percent of women with PTSD meeting the criteria for alcohol abuse. For people with co-occurring PTSD and substance abuse disorder, recognizing the signs of the disorders is the first step to recovery.

Symptoms of PTSD
While people with PTSD can experience a variety of symptoms related to their condition, these symptoms can be broken down into three types. The first is re-experiencing symptoms.
Re-experiencing symptoms include flashbacks where an individual repeatedly relives the trauma that caused their PTSD, has bad or haunting dreams about the trauma and has frightening thoughts or ideas that can be triggered by environmental factors. These symptoms can also cause physical side effects, such as increased heart rate and sweating. These flashbacks, thoughts and dreams can also be extremely debilitating and may prevent people from leading a healthy lifestyle.
Individuals with PTSD may also experience avoidance symptoms. Individuals experiencing avoidance symptoms often stay away from people, places or things that may remind them of the traumatic event that caused their PTSD. Individuals with these symptoms can also feel “numb” or lose interest in things that were enjoyable to them in the past, feel a strong sense of guilt, depression and worry, and may have trouble remembering and addressing the past trauma. Avoidance symptoms can cause people to isolate and will often push people with a co-occurring substance use disorder deeper into substance use.
Struggling with PTSD and Addiction?Our recovery programs are designed to meet your individual needs.
Get Help Now
“I came home in 2006, but metaphorically I didn’t really come home,” Stefanovic said. “I was lost, and people close to me told me that I was different. I was completely isolated. I didn’t want to be around family, friends. I got an apartment and stuck to my bedroom.”
The final group of symptoms is hyperarousal symptoms. Individuals with these symptoms experience anxiety, are easily startled, feel tense or “on edge,” have difficulty sleeping, and may be unable to control their emotions. Stefanovic also experienced some of these effects.
“Everyone has their own symptoms, and my symptoms involved nightmares,” said Stefanovic. “I would have panic attacks for no good reason. I couldn’t sleep. I was afraid to sleep.”
The most serious side effects associated with PTSD, however, are suicide and suicidal thoughts. Research shows a strong positive correlation between PTSD and a high risk of suicide and suicidal thoughts. Combine this with a substance use disorder, which often leads to decreased inhibitions, and individuals with PTSD become highly
susceptible to suicide.

Causes of PTSD
An individual’s development of PTSD is affected by a number of factors that determine the severity of the condition. The root cause for all PTSD is a traumatic event.
Trauma affects every person differently, and the majority of individuals who live through traumatic events go through a period of recovery, usually about a month long, before mentally moving on from that event. People who develop PTSD, however, usually experience a trauma so severe that it changes the ability for their brain to properly process the results of the event. In
military veterans, for example, live combat involving death or injury can lead to the development of PTSD. For civilians, a car accident, child abuse or neglect, sexual assault or a physical attack may haunt someone long after the event.
Stefanovic’s PTSD was caused by the horrors of war. While in Afghanistan, he witnessed an elementary school bombing. Some of his fellow Marines died in battle. He said he went through the worst suffering of his life while overseas, and his return home wasn’t easy.
“I was living with a lot of grief and guilt,” Stefanovic said. “I had no closure.”
While traumatic events play a significant role in the development of PTSD, genetics also affect the development of the condition. Genes may make certain people more likely to develop PTSD, and people with a family member with PTSD have a higher risk of developing the condition as well. Although research is still being conducted, scientists have theorized that individuals who develop PTSD may lack the genetic proteins needed to form fear memories and the brain chemicals that help with the response to fear. It is generally believed these pre-existing biological factors play a role in an individual’s development of PTSD.
In addition to traumatic events and genetic factors, key areas of the brain also have an effect on an individual’s development of PTSD. Two areas of the brain in particular are believed to affect the development of PTSD: the amygdala, the area of the brain responsible for learning about fear, and the hippocampus, the area of the brain responsible for creating memories. Scientific evidence has shown that the amygdala can be hyperactive in people with PTSD. Evidence has also shown a loss of volume in the hippocampus in individuals with PTSD, which may be the cause of memory deficits associated with the disorder.
Further research has led scientists to the conclusion that it may be possible to predict PTSD development in individuals based on psychological and neurochemical responses of people who experience a traumatic event.
Military service members too commonly develop PTSD as a result of their active duty. Veterans of different wars experience varying rates of PTSD.
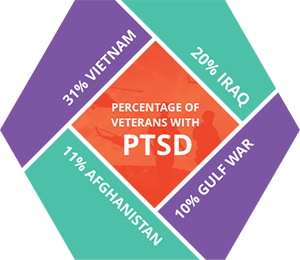
Civilian PTSD
Although the disorder is frequently associated with military veterans, PTSD among the general public is just as common. Civilian PTSD is caused by noncombat-related trauma that occurs in everyday life, such as car accidents, physical or sexual abuse, natural disasters or other harmful events. The trauma some individuals face can have a strong and lasting impact and potentially lead to PTSD development.
In the United States, 61 percent of men and 51 percent of women have experienced at least one traumatic event during their lifetime. Out of those who experience trauma, 8.1 percent of men and 20.4 percent of women develop PTSD. Rates of PTSD are also high among American youth, with a large number experiencing trauma before the age of 16.

Survivors of Sexual Assault
One of the most common traumatic events that cause PTSD is sexual assault, especially rape. Victims of sexual assault may experience PTSD symptoms such as repeated thoughts or memories of the assault, nightmares, avoidance symptoms, negative thoughts or feelings. According to the National Sexual Violence Resource Center, one in five women and one in 71 men will be raped during their lifetime. Female victims, which make up 91 percent of sexual assault victims, are most at risk for developing PTSD after an assault.
One study monitored PTSD symptoms among women who were raped for the first two weeks after the rape and found that 94 percent of those women experienced symptoms of PTSD during that time. Additionally, 30 percent of the studied group reported PTSD symptoms nine months later. According to the National Women’s Study, about 33 percent of rape victims develop PTSD at some point during their lifetime and 11 percent of rape victims currently suffer from PTSD.
- Seek medical attention immediately
- Call the police from the hospital
- Do not clean yourself after the assault
- Seek counseling and further help
Ready to Start Your Recovery?
Get a recovery plan that’s made for you.
Get Help Now
Childhood Trauma and Substance Abuse
Adults aren’t the only group that lives with PTSD. Children also experience trauma at high rates. Many adolescents suffering from PTSD turn to drugs to numb the physical, emotional and psychological pain of trauma.
Childhood PTSD
Anywhere from 15 to 43 percent of girls and 14 to 43 percent of boys in the United States experience a traumatic event, per the National Center for PTSD. Among this group, up to 15 percent of girls and up to 6 percent of boys have PTSD. Children who experience traumatic events grapple with a swirl of emotions. For example, sexually abused children often exhibit fear, worry, sadness and anger. They may also feel isolated or as though people are looking down on them. This can cause low self-esteem and an inability to trust others.
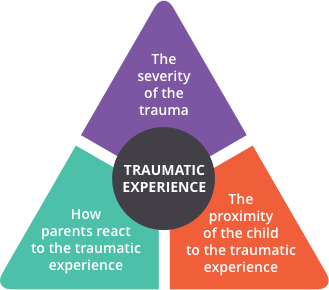
RISK FACTORS FOR PTSD IN CHILDREN
PTSD affects children in different ways. The more traumas a child experiences, the more likely he or she is to develop PTSD. Children and teens who go through intense traumas have the highest levels of PTSD symptoms.
Children ages 5–12 often do not have flashbacks or difficulties remembering their traumatic experience. Instead, they think there were signs that foretold the trauma and believe these signs may show up again. As a result, they stay cognizant of their surroundings to avoid future trauma.
Young children may also show signs of trauma in their play. For example, children who survive a school shooting may gravitate toward video games that involve shooting. They may even carry a gun to school themselves.
A teen may endure traumatic events, such as physical abuse, sexual assault, vehicular accidents or cyberbullying. Symptoms of PTSD among children ages 12–18 are similar to those found in many adults: aggressive behaviors, mood swings and isolation. Teens with PTSD may also self-harm or exhibit promiscuous behavior.
Substance Abuse as a Coping Mechanism
Looking for an outlet, many adolescents with PTSD turn to drugs or alcohol.
Overall, 25 percent of physically assaulted or abused teens reported lifetime substance abuse or dependence, per the survey.
Source: U.S. Department of Justice
According to a survey by the U.S. Department of Justice, 17 percent of boys who witnessed violence reported substance abuse or dependency. This statistic was similar to that of girls who witnessed violence.
The survey also found that 27.5 percent of sexually assaulted girls reported substance abuse or dependence in their lifetime. Among sexually assaulted boys, the number was 34.4 percent. Many of these children went on to commit delinquent acts, such as robbery or aggravated assault.
Overall, 25 percent of physically assaulted or abused teens reported lifetime substance abuse or dependence, per the survey.
A 2010 study published in the journal Addictive Behaviors found that PTSD contributes to the development of marijuana abuse or dependence among adolescents.
Another study, published in the journal Depression and Anxiety, found that PTSD led to alcohol, cocaine and marijuana use. The study found that levels of physical, sexual and emotional abuse in children were strongly associated with cocaine use later in life.

Treatment Options for PTSD and Substance Abuse Disorders
Traditionally, treatment experts have supported the notion that when treating co-occurring PTSD and substance abuse disorders, treatment for PTSD should not start until the individual has reached long-term sobriety. This line of thinking resulted from the notion that PTSD exposure therapy — treatment that forces individuals with PTSD to face the traumatizing event and subsequent fears —
may trigger relapse which can exacerbate their condition.
However, new research suggests the opposite.
45 percent of people with PTSD have a co-occurring substance use disorder.
Exposure therapy can greatly reduce symptoms of PTSD, even if an individual continues to use substances during exposure therapy. Studies have shown that going through treatment that forces these individuals to relive a painful event does not cause an increase in their substance use, nor does it cause a higher dropout rate from ordinary substance use disorder treatment.

Dual Recovery Programs
Treatment programs that focus on treating substance dependency and other mental health conditions called dual recovery programs provide users the opportunity to combat both co-occurring disorders simultaneously. Many PTSD and substance abuse disorder treatment programs differ in clinical approach but often improve an individual’s well-being either way.
According to the National Center for PTSD, cognitive behavioral therapy — talk-therapy in which patients work with a mental health counselor to help them become aware of negative or harmful thinking and how to properly respond to it — is the most effective way to treat PTSD. CBT is also used in a separate approach that combines the treatment with anxiety reduction techniques and coping skill development treatment.
Another treatment program called “COPE,” concurrently treats PTSD and substance use disorders through prolonged exposure to traumatic causes of an individual’s condition, relapse-prevention therapy and psychoeducation on PTSD Symptoms. Research has indicated that individuals who complete this treatment program experience improvement in
substance abuse habits and PTSD severity.
CBT is the most effective approach for treating children with PTSD. Trauma-focused CBT (TF-CBT) has been particularly effective in reducing childhood trauma. This approach involves talking to the child about his or her traumatic memory. From there, a mental health specialist teaches the child how to change problematic thoughts or beliefs about the trauma. The therapy technique helps children learn about the root of their distress at their own pace.
These treatments are almost always combined with a medication regimen to treat symptoms of the disorders and commonly use antidepressants, benzodiazepines, mood stabilizers and antipsychotic medications to improve an individual’s condition. Each of these programs is designed to have a positive impact on treating PTSD and substance abuse disorders.

Other Treatment Options
Some treatment professionals specialize in alternative forms of PTSD treatment, such as eye movement desensitization and reprocessing treatment.
EMDR therapy is an alternative form of PTSD counseling in which patients focus on stimuli such as eye movements, hand taps and sounds while discussing memories of their trauma, ultimately changing how a patient reacts to their traumatic memories.
Other alternative treatments include meditation, body work such as yoga, and creative activities including writing and making music. New treatment research is conducted constantly and as a result, treatment for PTSD is continuously evolving.
Some people don’t receive treatment until a court orders them to. Stefanovic ended up going to a drug court for veterans after an arrest. He was given the option of attending a residential rehab facility instead of incarceration. After months of rehab and therapy, he was able to recover from addiction. He still experiences some symptoms of PTSD, but he has developed healthy techniques for coping with those symptoms.

Types of PTSD
PTSD does not come in just one form. Various levels of responses and severity of PTSD exist for different individuals. Types of PTSD include:
Normal Stress Response
This type of PTSD usually occurs after an individual has experienced a single traumatic event. Individuals exhibit symptoms like bad memories, emotional numbness, dissociation from reality, isolation, and stress. Individuals experiencing this level of PTSD usually recover within a few weeks to a month.
Acute Stress Disorder
More common among individuals who experience prolonged exposure to trauma or traumatic events, acute stress disorder may cause panic attacks, confusion, dissociation, paranoia, insomnia, inability to care for themselves, and failure to maintain work and everyday life responsibilities.
Complex PTSD
Also known as Disorder of Extreme Stress, complex PTSD usually occurs among individuals exposed to prolonged trauma, such as children who were sexually abused. Individuals with complex PTSD commonly battle antisocial personality disorder and other dissociative disorders. Individuals with complex PTSD experience difficulty controlling their behaviors, emotions, and mental stability and often exhibit side effects of impulsivity, aggression, sexual deviance and substance use disorders.
Uncomplicated PTSD
Characterized by long-term re-experiencing symptoms of the traumatic event, avoidance of stimuli and triggers that remind an individual of trauma, emotional numbing, and increased arousal, this type of PTSD is the most commonly known type of PTSD, although it is not the most common type of PTSD among individuals with the disorder.
Comorbid PTSD
More common than uncomplicated PTSD, comorbid PTSD refers to PTSD that occurs simultaneously with another mental disorder like
depression, anxiety disorders and substance use disorders. Treatment for comorbid PTSD is most effective when the co-occurring disorders are treated together, particularly when the co-occurring disorder is a substance use disorder. Treatments used for uncomplicated PTSD should also be incorporated for people with comorbid PTSD, in addition to treatment for the separate mental disorder.
Getting HelpIf you or a loved one has experienced a trauma or event that affects your day-to-day activities, a substance use disorder, or any of the symptoms stated above, dual recovery treatment could be the answer. Seeking treatment can not only
help you overcome a substance use disorder but also help treat co-occurring PTSD and address the root causes of the disorders.
Get Help Now
PTSD Resources
-
PTSD Foundation of America
PTSD Foundation of America aims to bring healing to the military community with PTSD through counseling and peer mentoring. The nonprofit is also dedicated to raising awareness for PTSD through public events, social media, service organizations and churches and looks to bring resources together to meet the needs of military families.
-
The National Center for PTSD
The National Center for PTSD looks to help veterans who experience trauma. The center establishes this through research, education and treatment of PTSD and other stress-related symptoms. The center carries out psychotherapy studies, providing clinicians with science-based approaches to treatment.
-
Military with PTSD
Military with PTSD is an organization dedicated to helping military members with PTSD. The nonprofit educates veterans, caretakers and civilians on the effects PTSD has on numerous groups, including family members of veterans.
-
PTSD Alliance
PTSD Alliance is an organization dedicated to raising awareness for people with PTSD. The alliance provides medical professionals, support groups and counselors with up-to-date information on PTSD to help people overcome this disorder. Its website provides information on PTSD, including symptoms and common myths associated with the disorder.
-
Anxiety and Depression Association of America
Anxiety and Depression Association of America is an international organization that aims to prevent, treat and cure mental health disorders, including anxiety, depression and PTSD. The nonprofit offers information on PTSD — including facts, statistics and resources — on its website.
-
American Foundation for Suicide Prevention
About 20 veterans commit suicide each day, according to the United States Department of Veterans Affairs.
The American Foundation for Suicide Prevention looks to raise awareness and funds for scientific research to aid those affected by suicide. It also provides suicide-prevention resources.
-
Sidran Traumatic Stress Institute, Inc.
Sidran Traumatic Stress Institute, Inc. is an organization dedicated to helping people understand, recover from and treat PTSD, including co-occurring disorders such as addiction. The nonprofit accomplishes this through educational programming, publications and resources.
-
Operation: Warrior’s Path
Operation: Warrior’s Path is an organization that strives to help veterans overcome PTSD. The nonprofit, led by veterans, offers equine therapy and other nonconventional treatment approaches to assist those with PTSD. Also, its Warrior’s Project builds or repairs homes for veterans.
-
PTSD United
PTSD United is a nonprofit that offers support and resources for those with PTSD, their families and caregivers. The organization provides statistics on PTSD, resources and a 24/7 anonymous online community.
 Addiction
Addiction
 Treatment
Treatment
 Faith & Religion
Faith & Religion
 Active Recovery
Active Recovery
 Our Community
Our Community









